Endoscopic Discectomy is a minimally-invasive procedure to relieve pain, numbness, or weakness caused by herniated discs pressing on nerve roots or the spinal cord. Call Downtown Pain Physicians today and schedule an appointment with our pain management specialist. Our physicians offer comprehensive, personalized, and time-tested treatments that focus on your specific level of pain.
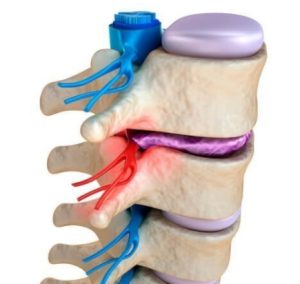
Patients who experience back problems related to spinal discs experience intense pain. Conditions such as sciatica can cause referred pain in the legs or low back pain. These conditions can be very difficult to find pain relief from using more conservative treatment options or pain management injections.
Downtown Pain Physicians in New York, NY offers multiple pain options to patients who are looking to achieve lasting pain relief. This includes endoscopic procedures like endoscopic discectomy. Surgery is something that most patients want to avoid because of its long recovery time, invasiveness, and the pain involved. Endoscopic discectomy is different. It uses minimally invasive techniques to remove disc material that causes pain.
Before the pain medicine specialists at Downtown Pain Physicians recommend any treatment, they evaluate each patient and look at their past medical history to determine what treatments have the best chance of providing significant or permanent pain relief for the condition that causes it.
We work with each patient to find a pain treatment that will relieve or provide them with lasting pain relief during our initial consultation and pre-procedure visits. Downtown Pain Physicians will not recommend treatment to a patient unless we have evidence that indicates that treatment has the potential to be successful.
Endoscopic Discectomy in Downtown Brooklyn & Lower Manhattan
An endoscopic discectomy is a procedure that removes herniated disc material from the spine in an outpatient setting. The herniated disc material is removed using a probe with a hollow center. The procedure is minimally invasive and uses a keyhole incision to get to the spine.
An endoscope is a stiff or flexible tube that has a camera on the end of it. It helps the orthopedic surgeon see the disc and the structures related to it. With the help of the camera, the doctor can remove the parts of the disc that need to be removed.
Traditional spinal surgery involves cutting through muscle and other tissue to get to the spine. This is a more invasive surgery that causes more pain and a longer recovery time. In an endoscopic discectomy, the muscle and tissues are separated using dilation tubes. They also help the doctor see the entire field.
What are Spinal Discs?
Spinal discs are the cushions that sit in between the individual bones in the spine, also known as vertebrae. When someone has a problem with one of their discs, it may have slipped out or herniated from its position between the bones. Once this occurs, the disc starts rubbing against the spinal nerve. This can cause feelings of weakness, pain, or numbness in your arms or legs. Problems with spinal discs can occur in any part of the spine, but it is most common in the lower back. This is called the lumbar spine.
What is Endoscopic Discectomy Used to Treat?
Endoscopic Discectomy is used to treat disc-related problems such as:
Lumbar Spinal Stenosis:
Spinal stenosis causes the spine to narrow around the neural elements in the spine. These include the nerve roots and spinal cord. This can cause disc herniation as well as arthritis. Once arthritis begins to occur along with aging, the intervertebral discs or discs in between the vertebrae begin to narrow. Narrow space means that the nerves don’t have the space they should have to branch out from the spine. This can cause bone spurs to form, which prevents movement from occurring at the joint. They can cause nerve compression through ligament growth or simply pressing against it.
Spondylolisthesis:
Spondylolisthesis is a condition where the vertebra of the spine slips backward or forwards. While this condition can be caused by multiple issues, it results in the nerve roots being pressed down on due to the vertebrae of the spine being put into an abnormal position. This condition can also alter the size of the spinal canal or the vertebral space known as the foramen where the spinal nerves go out and into other parts of the body.
Lumbar Pinched Nerves:
This refers to nerves that have been compressed due to conditions like disc herniation or spinal stenosis.
Scoliosis: Scoliosis refers to a sideways curvature of the spine. It puts pressure and stress on joints like the shoulders or hips. Since it can lead to degenerative changes, this condition may put stress on the discs in between the vertebrae.
Lumbar Facet Joint Syndrome:
The facet joints, known as zygapophysial joints, or Z-joints, are pairs of bone structures located on the back of each spinal vertebra or spinal column bone. These bones work together to let movement occur between two vertebrae. A capsule surrounding the facet joints keeps them bathed in lubricating fluid. Other joints in the body such as shoulder or knee joints work similarly. When this fluid starts to get low due to lack of cartilage, bone spurs begin to form and this can cause nerve compression directly or joint inflammation.
“VERY KIND”
Dr. Raval is very kind and explains everything in layman’s terms, which is super helpful. Thanks so much, guys! 🙂
“PLEASANT AND PROFESSIONAL”
Best doctor visit I ever had. Staff was pleasant and the doctor was very pleasant and professional. Took his time and answered all my questions.
Symptoms of Disc Issues
When patients have issues with their spinal discs, they will start to experience symptoms that will vary depending on where the disc is and if it’s pressing on a nerve or not. Some patients can have a herniated disc and not know until they have a spinal image taken.
Pain in the arms or legs from a disc that has been damaged or moved will be concentrated in the calf, buttocks, and thigh. Pain in part of the foot is also a common symptom. For patients who have a herniated disc in their neck, they will feel pain in their shoulder or arm. It may also travel into the arm or leg when coughing, sneezing, or moving into different positions. It may present as sharp or burning pain.
Numbness and tingling are another common symptoms of disc slippage. It may radiate in the affected body part. Patients can also experience muscle weakness that makes it difficult to lift or hold objects due to the nerves that help those muscles weakening.
Risks and Causes of Disc Problems
Patients experience disc herniation for different reasons including injury caused by lifting something heavy with their back instead of their knees and in some cases a herniated disc can be caused by trauma.
Risks such as weight, occupation, and genetics can lead to an increased risk for disc problems.
Who is a Good Candidate for Endoscopic Discectomy?
Book Appointment
212.404.8070An endoscopic discectomy is a procedure that benefits patients who:
- Have had testing such as a myelogram, MRI, or CT that shows a herniated disc.
- Symptoms that haven’t improved using physical therapy.
- Significant numbness, pain, or weakness in the leg or foot
- Loss of bowel or bladder control, leg weakness, or loss of feeling in the genital area.
Why Choose This Procedure?
The choice to have an endoscopic discectomy depends on the individual patient. If you have not tried other treatment options, the doctor may recommend those first before having this procedure. He will also go over the risks and benefits of having it if you decide that you are interested in this treatment option.
Preparing for an Endoscopic Discectomy
Before surgery, you will undergo some tests like a chest x-ray, blood test, and echocardiogram. You’ll also fill out forms and give consent related to your medical history. This will cover areas such as:
- Previous surgeries
- Bleeding history
- Reactions to anesthesia
- Allergies
- Medications and vitamins being taken
It’s important to note that all medications, vitamins, and supplements that you take need to be disclosed to the doctor, even over-the-counter medications.
Depending on the types of medication you are taking, some may need to be discontinued temporarily. These types of medication include:
- Naprosyn
- Advil
- Motrin
- Nuprin
- Aleve
- Plavix
- Coumadin
They need to be discontinued 1-2 weeks before surgery as directed by the doctor. In addition, do not smoke, chew tobacco or drink alcohol the week before and 2 weeks following surgery. These things do increase your risk for bleeding problems.
Don’t eat or drink past midnight on the day of the surgery.
Before coming in on the day of the procedure, make sure to arrange for someone to drive you home. The anesthesia and pain medicine used as part of the procedure makes driving unsafe.
On the day of the procedure, make sure to shower using antibacterial soap, remove any makeup, contacts, nail polish, or hairpins. If you are taking medications that day, take them with small sips of water. Make sure to bring your current list of medications with you to the procedure and any food or medication allergy information with you.
What Happens During the Procedure?
On the day of your procedure, make sure to arrive an hour before your scheduled procedure. During this time, you will complete any pre-procedure paperwork and the doctor will go over the risks and effects of anesthesia. You’ll have an IV placed in your arm and the surgery should take between 1 and 2 hours.
You will lay on your back and be given the anesthesia which will make you fall asleep. After this, you’ll be rolled onto your stomach to expose your spine. The doctor will prepare and clean the area where the incision will be made. Before making the incision a needle will be inserted into the spine with the assistance of a fluoroscope. It helps identify where the problem with the vertebrae and disc is.
The incision itself is about 1-inch long. Muscles in the area will be moved using what are known as dilator tubes, creating a tunnel to the problem area of the spine. A guidewire is inserted through the tube and the doctor will make a hole using a drill in the lamina. It’s a bony covering. The doctor will locate the spinal disc with a microscope and take out the damaged or exposed portions only. Any bone spurs found during the procedure will also be removed.
Once the removal is complete, the instruments used for the procedure are taken out and the incision will be closed. Since you will be asleep for the procedure, you shouldn’t feel anything until you wake up.
What Happens After the Procedure?
You’ll wake up in a post-procedure recovery room. Your blood pressure, respiration, and heart rate will be monitored. Once you can gradually start moving around, you’ll be able to go home the same day.
Post-Procedure Care
Wait for two days before attempting to shower. Don’t take a bath because the incision area shouldn’t be submerged in water completely. Expect some drainage from the wound.
Limit any lifting, twisting, or bending for six weeks following the procedure. Anything you do lift should be no more than 5 pounds in weight. Avoid participating in any strenuous activities like yard work, sex, or housework.
Don’t drive for the first two weeks after the surgery or per the doctor’s instructions. Avoid drinking alcohol as well during this time frame,
especially if you are taking narcotic medications.
Get up and walk for 5 to 10 minutes every 3 to 4 hours and increase the time as you can do so. You may need help with activities such as bathing or dressing for the first few days.
Recovery Time
The recovery time for the procedure ranges from 1 to 4 weeks depending on the reason for the procedure and overall health. Expect to feel pain at the incision site. Pain may not be relieved immediately through surgery. Do any physical therapy exercises prescribed to help aid in your recovery.
Patients usually return to work within 2 to 4 weeks. For those with more physically demanding jobs expect to return 8 to 12 weeks after their procedure.
Risks and Side Effects
As with any procedure, there may be side effects. Make sure the drainage from the incision doesn’t turn yellow or green. If it does, notify the doctor immediately. Other risks include:
- Blood clots
- Anesthesia reaction
- Infection
- Deep Vein Thrombosis (DVT blood clots)
- Lung problems
- Nerve damage
- Persistant Pain
Any problems on this list are considered urgent, and you should contact or office or seek treatment at the hospital if they develop.
Results of Endoscopic Discectomy
80% of patients in a study conducted over a 10-year period had excellent results after the procedure.
90% of patients studied over an average of 2 years after surgery had excellent results post-procedure.
38 out of 62 patients followed after this procedure required no further surgery.
1 year after the procedure, patients reported their pain relief at 71%.
Frequently Asked Questions
What are the Benefits of Endoscopic Discectomy?
There are several benefits to endoscopic discectomy including :
- No large incision
- Uses a local anesthesia injection
- Short recovery
- Reduced risk of complications such as anesthesia reactions, infection, blood loss, and scaring
- No bone fusion or bone removal
- The disc remains intact
- High rate of success
- Procedure completed outpatient
What is Failed Back Surgery Syndrome? (FBSS)
This refers to back spine surgery that has failed to provide pain relief. Open spine procedures fail about 20 to 40% of the time, which is why an Endoscopic Discectomy is an option before this stage.
Will my Bulging or Herniated Disc be Removed?
This procedure removes the part of the disc that is exposed.
What are the Types of Endoscopic Discectomy Procedures?
Endoscopic lumbar discectomy and endoscopic cervical discectomy.
What are the Risks of Endoscopic Discectomy?
The risks of Endoscopic Discectomy are rare but still something to consider. They include bleeding, infections, failure to relieve pain, and spinal cord and nerve injuries.
What if Endoscopic Discectomy Does Not Relieve My Pain?
If the procedure does not offer the level of pain relief you expect, there are other options. This is also why Downtown Pain Physicians goes through such a thorough consultation process. We look at your past medical history, the procedures you’re had, and the medications you take to help determine which treatment options have the best chance to provide lasting pain relief.
Your NYC Spine Pain Specialists
As the best pain management doctors in NYC, Downtown Pain Physicians want to help you relieve your chronic spinal pain with procedures like an Endoscopic discectomy. If you’re searching for a pain management solution that will alleviate your pain, call us at 212-404-8070 to schedule your consultation appointment.
Call Downtown Pain Physicians today and schedule an Endoscopic Discectomy appointment with our specialist. A minimally-invasive procedure is performed through a small tubular device. It is designed to relieve pain, numbness, or weakness caused by herniated discs pressing on nerve roots or the spinal cord.
Do you have any questions about Endoscopic Discectomy? Would you like to schedule an appointment with the best pain specialist in Brooklyn and Lower Manhattan, Dr. Raj Raval, MD? Please call our office for a consultation and indicate which location you want to visit.
Dr. Raj Raval, M.D.
- Interventional Pain & Musculoskeletal Medicine Specialist
Education & training
- SUNY Health Science Center
- Rutgers University Fellowship
Dr. Oryan Baruch, DO
- Board Certified
- Interventional Pain & Musculoskeletal Medicine Specialist
Education & training
- Doctor of Osteopathic Medicine, Touro College
- Fellowship – Spine & Sports Medicine, Rutgers

